Surgical Outcome Factors Checklist
Patient Evaluation Tool
Estimated Risk Profile
Recommended Priority Questions:
Pre-Op Success Boosters
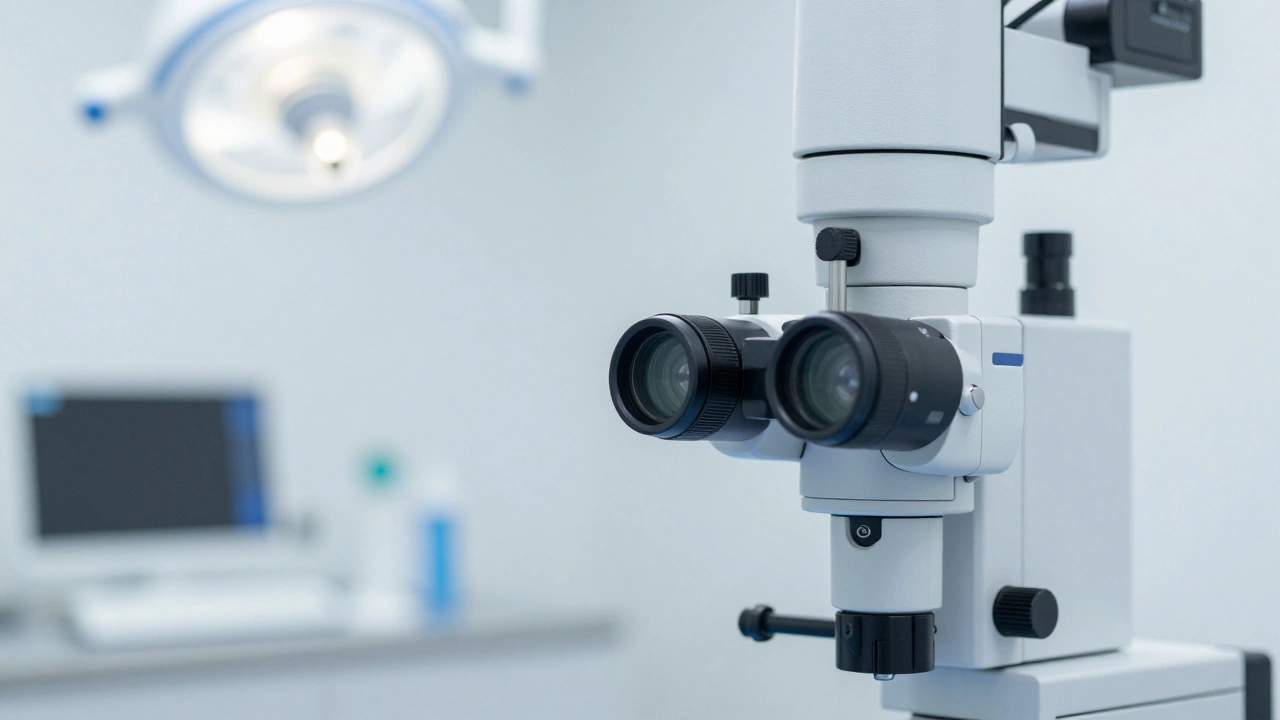
The High-Performers: Surgeries with Exceptional Outcomes
If we are looking at raw numbers, the surgeries with the highest success rates are typically those that are highly standardized, minimally invasive, and treat localized issues. For example, Cataract Surgery is widely considered one of the most successful procedures in the world. Because it involves replacing a cloudy lens with an artificial one, the technical process is predictable. Most patients experience immediate improvement in vision, and complication rates are incredibly low. Similarly, Appendectomy (removing the appendix) has a very high success rate because the goal is simple: remove the infected organ to stop the pain. Once the appendix is out, the primary problem is solved. These are "fix-it" surgeries where the pathology is clear and the solution is direct. However, success in these cases is often measured by "technical success" (did the surgery go as planned?). This is different from "functional success" found in orthopedics. For instance, a Total Hip Replacement has a high success rate in terms of joint stability and longevity-many implants last 20 years or more-but success for the patient is defined by whether they can walk without pain again. This makes the data a bit more subjective.Why Some Procedures Are Riskier Than Others
Not all surgeries are created equal. The success rate drops as the complexity of the organ system increases. A skin graft is relatively straightforward because skin regenerates well. Brain surgery, on the other hand, deals with an organ that doesn't regenerate and where a millimeter of error can change a person's personality or speech capabilities. Cardiovascular Surgery, such as a CABG (Coronary Artery Bypass Graft), has a high success rate in terms of saving lives, but it carries a higher risk of immediate complications like stroke or infection compared to a simple gallbladder removal. The risk is tied to the criticality of the organ; if the heart stops during a procedure, the window for recovery is seconds, not hours. Another factor is the patient's baseline health. A 25-year-old with no comorbidities will have a vastly different success probability for a Cholecystectomy (gallbladder removal) than an 80-year-old with diabetes and kidney disease. This is why surgeons provide "personalized risk profiles" rather than just quoting a general percentage from a textbook.Private Surgery Cost vs. Outcome Quality
When you move from public healthcare to the private sector, you aren't necessarily paying for a "higher success rate" in terms of the medical result-the biological reality of the surgery remains the same. What you are paying for is the environment, the speed of access, and the level of personalization. In private care, private surgery cost covers things like a private room, a choice of consultant, and often a more tailored rehabilitation plan. While the surgical technique (the "how") is often identical to what you'd get in a public hospital, the "around-the-surgery" care can influence the perceived success. Better post-operative physiotherapy, for example, can make a joint replacement feel more successful because the recovery is managed more aggressively.| Procedure Type | Primary Success Metric | Relative Risk Level | Typical Recovery Focus |
|---|---|---|---|
| Ophthalmic (Cataracts) | Visual Acuity | Very Low | Quick healing, drop administration |
| Orthopedic (Hip/Knee) | Mobility & Pain Reduction | Low to Moderate | Intensive physical therapy |
| Gastrointestinal (Gallbladder) | Symptom Resolution | Low | Dietary adjustment, short rest |
| Cardiac (Bypass) | Long-term Survival | High | Cardiac rehab, lifestyle change |
How to Actually Measure Success Before You Book
If you are trying to figure out if a specific surgery is "successful," stop looking at the average percentage and start asking specific questions. A "90% success rate" is meaningless if you don't know how the surgeon defines success. Does it mean the patient survived? Or does it mean the patient returned to work within six weeks? Ask for the "complication rate" instead. This tells you how often things go wrong, which is often more useful than knowing how often they go right. For example, if a surgeon says a procedure is 95% successful, but 10% of patients experience a chronic infection, that's a crucial detail. Moreover, look for Patient-Reported Outcome Measures (PROMs). These are standardized surveys where patients rate their own quality of life after surgery. This is the gold standard for understanding if a surgery actually improved a life, rather than just fixing a biological problem on a scan.Common Pitfalls in Evaluating Surgical Options
One of the biggest mistakes patients make is assuming that the most expensive surgeon or the fanciest private clinic guarantees the highest success rate. Success is more closely linked to the "volume」 of the surgeon-how many times they have performed that specific procedure. Research consistently shows that high-volume surgeons (those who do hundreds of the same operation per year) have lower complication rates than those who do a variety of different surgeries. This is the "practice makes perfect" rule of medicine. If a surgeon does five heart valves a year and fifty hip replacements, they are likely more "successful" at the latter. Another trap is ignoring the "downside risk." Every surgery has a trade-off. You might achieve a 100% success rate in removing a tumor, but if the success comes at the cost of permanent nerve damage, was the surgery a total success? Always ask about the "functional cost" of the procedure.Steps to Maximize Your Own Surgical Success
Regardless of the procedure, you have a role in the success rate. Surgery is the catalyst, but recovery is where the actual result is solidified.- Pre-habilitation: Don't just wait for the surgery. If you're getting a knee replacement, strengthening the surrounding muscles before the operation can significantly improve the outcome.
- Smoking Cessation: Nicotine constricts blood vessels and slows healing. Quitting even two weeks before surgery can drastically reduce the risk of wound infections.
- Managing Expectations: Understand the difference between "cured" and "improved." If you expect a surgery to make you feel 20 years younger, you might perceive a successful medical result as a failure.
- Strict Adherence to Aftercare: The most successful surgeries can fail if the patient ignores the post-op movement restrictions or forgets their blood-thinners.
The Future of Surgical Outcomes
We are moving toward an era of "precision surgery." With the rise of Robotic Surgery and AI-driven planning, the margin of error is shrinking. Robots don't have hand tremors, and they allow for smaller incisions, which means less blood loss and faster healing times. This is pushing the success rates of complex abdominal and urological surgeries higher than they ever were with traditional open surgery. Additionally, the use of Big Data in healthcare allows hospitals to track outcomes in real-time. We no longer rely on a surgeon's "gut feeling" about their success rate; we have digital registries that track every patient's progress for years. This transparency makes it easier for you to find a provider with a proven track record of excellence.Does a higher price for private surgery mean a better success rate?
Not necessarily. The cost of private surgery primarily covers amenities, speed of access, and a more personalized experience. While private surgeons are often highly experienced, the biological success of the surgery depends more on the surgeon's volume of experience and the patient's health than the price of the hospital room.
What is the most successful type of surgery overall?
In terms of predictable, positive outcomes with very low risk, cataract surgery and simple appendectomies are among the most successful. These are standardized procedures with clear goals and low complication rates.
How can I find out a surgeon's personal success rate?
You should ask the surgeon directly about their "volume" (how many of this specific procedure they do per year) and their personal complication rates. Ask them to define what they consider a "success" for your specific case and if they have data from Patient-Reported Outcome Measures (PROMs).
Can a surgery be a technical success but a personal failure?
Yes. A surgeon may successfully remove a gallbladder or repair a ligament (technical success), but if the patient is still in pain or cannot return to their desired activity level, the patient may view the surgery as a failure. This is why aligning expectations before the operation is critical.
Which factors most influence surgical success?
The most critical factors include the surgeon's experience level (volume), the patient's overall health (age, weight, and comorbidities like diabetes), the type of anesthesia used, and the quality of post-operative rehabilitation.