Nerve Pain Treatment Planner
Select your primary symptoms below to generate a personalized treatment overview based on clinical guidelines.
Recommended Multimodal Approach
Suggested Combination Stack
Why this works
Important Considerations
Disclaimer: This tool provides educational information based on general medical guidelines. It does not replace professional medical advice. Always consult your healthcare provider before starting new medications.
That burning, shooting, or electric-shock sensation is not just "pain." It’s a signal that your nervous system has misfired. If you are dealing with neuropathic pain, standard over-the-counter painkillers like ibuprofen or acetaminophen often do nothing. They target inflammation, but nerve damage operates on a different frequency. So, what is the strongest pain relief for nerve pain? The answer isn’t a single pill; it is a combination of specific prescription medications, targeted therapies, and sometimes surgical intervention.
For most people, the "strongest" relief comes from medications that calm down hyperactive nerves rather than block pain signals at the source. We will break down the top-tier pharmaceutical options, the emerging treatments available in 2026, and the non-drug approaches that can actually change how your brain processes pain.
The Gold Standard: Anticonvulsants
When doctors talk about treating nerve pain, they rarely start with opioids. Instead, they reach for anticonvulsants. These drugs were originally designed to stop seizures, but they have a side effect that is perfect for nerve pain: they stabilize the electrical activity in your nerves. Think of your damaged nerve as a short-circuiting wire sending random sparks. Anticonvulsants act like insulation, stopping those sparks before they reach your brain.
Gabapentin (Neurontin) is often the first line of defense. It works by binding to calcium channels in the central nervous system, reducing the release of neurotransmitters that transmit pain signals. It is particularly effective for postherpetic neuralgia (shingles pain) and diabetic neuropathy. However, it requires careful dosing. You usually start low and go slow, increasing the dose every few days until you find relief or hit side effects like dizziness or fatigue.
If Gabapentin doesn’t cut it, Pregabalin (Lyrica) is often the next step. It works similarly but is absorbed faster and more predictably by the body. Many patients report that Pregabalin provides stronger relief with fewer fluctuations in blood levels. It is also FDA-approved for fibromyalgia and spinal cord injury pain. The trade-off? It carries a higher risk of weight gain and dependency compared to some other options.
Antidepressants That Don’t Treat Depression
This sounds counterintuitive, but certain antidepressants are powerful tools for nerve pain. Specifically, we are talking about SNRIs (Serotonin-Norepinephrine Reuptake Inhibitors) and TCAs (Tricyclic Antidepressants). These drugs increase the levels of serotonin and norepinephrine in your spinal cord. These chemicals help dampen the transmission of pain signals up to the brain.
Duloxetine (Cymbalta) is an SNRI that is widely considered one of the most effective medications for chronic musculoskeletal pain and diabetic peripheral neuropathy. Unlike older antidepressants, Duloxetine tends to have fewer sedative effects, making it easier to take during the day. Studies show it can reduce pain intensity by 30-50% in many patients within four to eight weeks.
On the TCA side, Amitriptyline is a classic choice. It is cheap, effective, and has been used for decades. However, it comes with a heavy list of side effects, including dry mouth, constipation, and significant drowsiness. Because of this, it is often prescribed at night to help with sleep while treating pain simultaneously. For many older adults, the cognitive fog associated with Amitriptyline makes it less desirable than newer options.
Topical Treatments: Localized Relief
If your nerve pain is localized-say, only in your feet or along a specific patch of skin after shingles-you might not need systemic medication. Topical treatments deliver high concentrations of pain-relieving agents directly to the site without affecting the rest of your body.
- Lidocaine Patches: These contain a local anesthetic that numbs the area. They are excellent for postherpetic neuralgia. You apply them directly over the painful spot for 12 hours a day. The relief is immediate but temporary.
- Capsaicin Cream: Derived from chili peppers, capsaicin depletes Substance P, a chemical involved in transmitting pain signals. It takes several weeks of daily use to see results, and it burns initially. However, for long-term management of diabetic neuropathy, it can be highly effective.
- High-Dose Capsaicin Patch (Qutenza): This is a clinical treatment applied by a healthcare provider. It delivers a much higher concentration than over-the-counter creams, providing relief that can last up to three months.

When Oral Meds Fail: Interventional Procedures
If medications provide less than 50% relief, or if side effects are unmanageable, you move to interventional procedures. These are not cures, but they can significantly reduce pain intensity.
Nerve Blocks involve injecting a local anesthetic, sometimes combined with a steroid, directly around the affected nerve. This can provide temporary relief ranging from weeks to months. It helps diagnose which nerve is causing the pain and can break the cycle of chronic pain signaling.
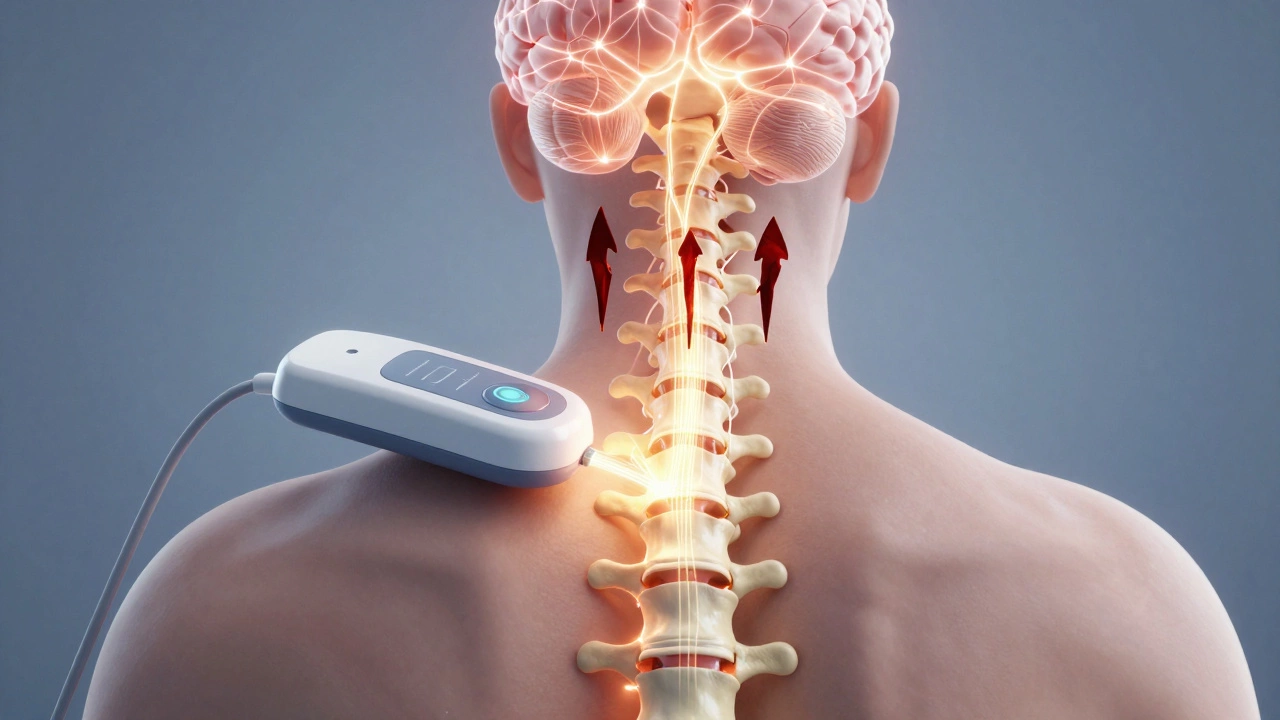
For more severe cases, Spinal Cord Stimulation (SCS) is a game-changer. A small device is implanted under the skin, sending mild electrical pulses to the spinal cord. These pulses interfere with pain signals before they reach the brain. Modern SCS devices use "burst" patterns or high-frequency stimulation that don’t cause the tingling sensation of older models. Success rates vary, but many patients report a 70-80% reduction in pain.
Emerging Therapies and Supplements
In 2026, the landscape of nerve pain treatment is expanding beyond traditional pills. While supplements are not "strong" in the same way prescription drugs are, they can support nerve health and enhance the effectiveness of other treatments.
Alpha-Lipoic Acid is an antioxidant that has shown promise in treating diabetic neuropathy. European guidelines recommend it as a standard treatment. It helps reduce oxidative stress in the nerves, which may slow further damage. Typical doses range from 600mg to 1200mg daily.
Vitamin B12 deficiency is a common cause of nerve damage. If your levels are low, supplementation can reverse symptoms. Methylcobalamin, the active form of B12, is preferred for nerve repair. Always get your levels tested before supplementing heavily.
Newer research is also looking into Ketamine infusions for refractory nerve pain. Ketamine blocks NMDA receptors in the brain, which play a key role in chronic pain sensitization. A series of infusions can provide relief for months, though it is typically reserved for cases where all other options have failed.
Comparison of Common Nerve Pain Treatments
| Treatment | Best For | Strength Level | Common Side Effects |
|---|---|---|---|
| Gabapentin | Shingles pain, general neuropathy | Moderate | Dizziness, fatigue, brain fog |
| Pregabalin | Fibromyalgia, spinal injury | Strong | Weight gain, drowsiness, dependency |
| Duloxetine | Diabetic neuropathy, musculoskeletal pain | Moderate to Strong | Nausea, dry mouth, insomnia |
| Lidocaine Patch | Localized pain (feet, shingles) | Mild to Moderate | Skin irritation, redness |
| Spinal Cord Stimulator | Severe, refractory pain | Very Strong | Surgical risks, infection, lead migration |
The Role of Lifestyle and Mental Health
You cannot out-medicate a stressed nervous system. Chronic nerve pain keeps your body in a state of high alert, which amplifies pain signals. This is why psychological therapies are now considered part of the "strongest" treatment plans.
Cognitive Behavioral Therapy (CBT) for pain doesn’t mean the pain is "in your head." It means learning how to change your reaction to pain. By reducing fear and anxiety around pain, you lower the volume of the signal your brain receives. Studies show that CBT can improve function and quality of life even if pain scores remain unchanged.
Physical activity is also crucial. Gentle movement, such as walking or swimming, improves blood flow to the nerves and prevents muscle weakness. Avoid complete rest, which can lead to deconditioning and make pain worse.
What About Opioids?
Opioids like oxycodone or morphine are generally not recommended for long-term nerve pain treatment. They are effective for acute injury pain but have limited efficacy for neuropathic pain. More importantly, they carry a high risk of tolerance, dependence, and overdose. Long-term use can actually worsen nerve pain through a condition called opioid-induced hyperalgesia, where your nervous system becomes more sensitive to pain over time.
If you are currently taking opioids for nerve pain, work with your doctor to taper off gradually. Switching to a combination of Gabapentin and Duloxetine often provides better relief with fewer risks.
Finding Your Right Combination
The "strongest" pain relief is rarely one thing. It is usually a combination. For example, many patients find success with a low dose of Gabapentin at night, Duloxetine during the day, and Lidocaine patches on the worst areas. This multimodal approach attacks pain from multiple angles: calming the nerves, blocking signal transmission, and numbing the surface.
It takes time to find the right mix. Keep a pain diary to track what works. Note the dosage, timing, and any side effects. Share this with your doctor so you can adjust the plan efficiently. Remember, the goal is not necessarily zero pain, but functional improvement-the ability to sleep, work, and enjoy life despite the discomfort.
Is there a cure for nerve pain?
There is no universal cure for nerve pain because it depends on the underlying cause. If the nerve damage is due to a vitamin deficiency or compression, treating that cause can resolve the pain. However, for conditions like diabetic neuropathy or idiopathic neuropathy, the focus is on managing symptoms and preventing further damage rather than curing the condition entirely.
Which is better for nerve pain: Gabapentin or Pregabalin?
Pregabalin is often considered more potent and predictable than Gabapentin because it has higher bioavailability. However, Gabapentin is cheaper and may have a slightly lower risk of certain side effects. The best choice depends on individual response, cost considerations, and specific medical history. Many doctors start with Gabapentin and switch to Pregabalin if needed.
Can nerve pain go away on its own?
In some cases, yes. If the nerve injury is minor and the underlying cause is removed (e.g., releasing pressure on a nerve), the pain may resolve as the nerve heals. However, chronic nerve pain lasting more than six months is unlikely to disappear without treatment. Early intervention improves the chances of recovery.
Are there natural remedies for nerve pain?
While no natural remedy replaces prescription medication for severe nerve pain, some supplements can help. Alpha-lipoic acid, Vitamin B12, and Magnesium have evidence supporting their use for nerve health. Turmeric and omega-3 fatty acids may reduce inflammation. Always consult your doctor before starting supplements, as they can interact with medications.
How long does it take for nerve pain medication to work?
It varies by medication. Topical treatments like Lidocaine work immediately. Gabapentin and Pregabalin may take a few days to a week to show initial effects, with full benefits appearing after several weeks of consistent use. Antidepressants like Duloxetine often take 4 to 8 weeks to reach maximum efficacy. Patience and consistent dosing are key.




