Opioid Potency Comparison Tool
About the Comparison
This tool visualizes the concept of "Morphine Milligram Equivalents" (MME). Since different drugs bind to receptors with varying efficiency, 1mg of Fentanyl provides significantly more pain relief than 1mg of Morphine.
Use this to understand why doctors switch patients between medications or change dosages carefully. Higher potency does not always mean "better"—it requires precise measurement to avoid toxicity.
How this compares to other drugs:
The Reality Behind the Strongest Painkillers
When patients face excruciating discomfort, the question often arises about which medication offers the highest level of relief. In medical terms, there is no single universal champion for pain relief, but the hierarchy of strength is well-established among healthcare providers. The medications classified as severe pain medication typically belong to a specific class known as high-potency opioids. These drugs interact directly with the brain's opioid receptors to block pain signals. However, potency comes with significant responsibility regarding safety and regulation.
Doctors do not prescribe the strongest drug simply to achieve maximum numbness. Instead, they balance efficacy with the risk of side effects like respiratory depression. Understanding this balance is crucial for anyone navigating serious health conditions. We will explore the medications used for breakthrough pain, how they differ from standard treatments, and the safety protocols surrounding their use.
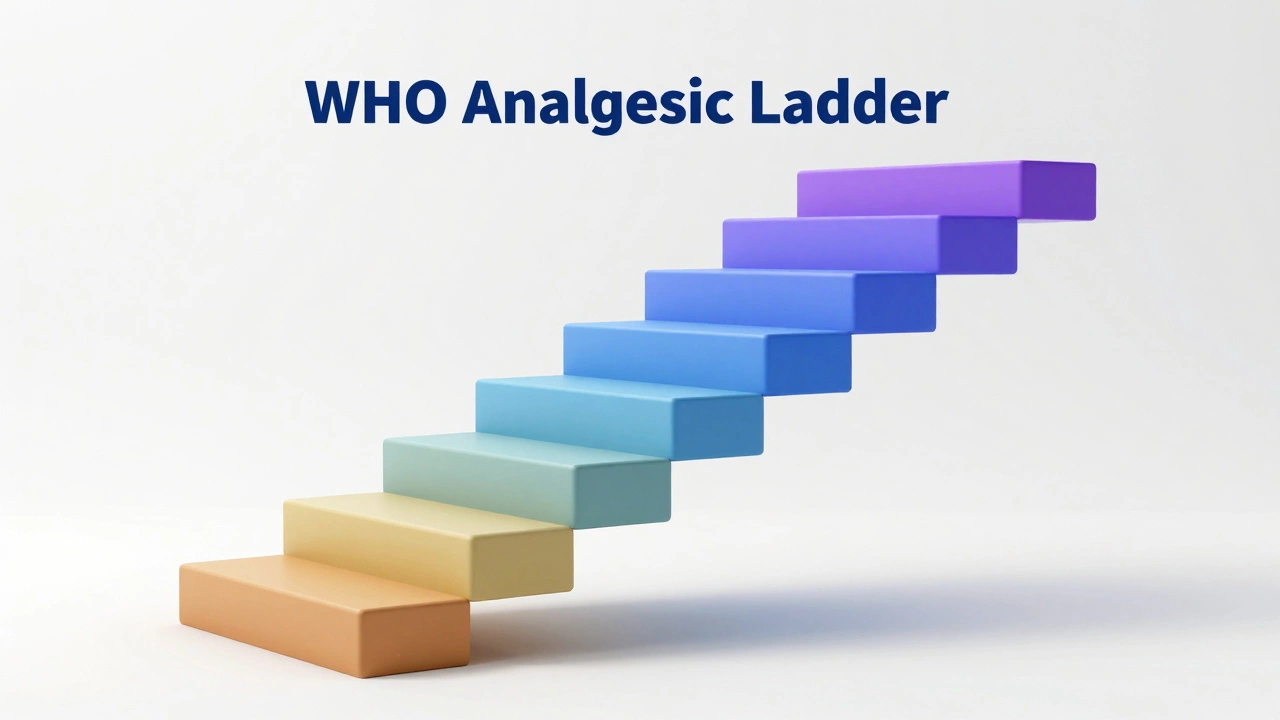
Mapping Pain Management Levels
To understand where the strongest medications fit, you need to look at the global standard for pain control. The World Health Organization established a framework known as the WHO Analgesic Laddera stepwise approach to cancer pain management developed by the World Health Organization. This system guides physicians from mild analgesics to powerful prescription drugs depending on symptom intensity.
At the bottom of the ladder, non-opioid analgesics handle mild discomfort. Common examples include acetaminophen or ibuprofen. When pain escalates beyond this threshold, weak opioids are introduced. Codeine or tramadol might be sufficient for moderate cases. Finally, for severe uncontrolled pain, the third step initiates strong opioids. This is where the conversation shifts to heavy-hitting medications like morphine equivalents and synthetic derivatives.
This tiered approach ensures patients aren't exposed to unnecessary risks early on. If mild interventions fail, moving up the ladder becomes medically necessary. Ignoring pain levels can lead to poor outcomes, affecting sleep, mobility, and mental health.
High-Potency Opioids and Their Profiles
Within the strongest category, several specific drugs stand out due to their molecular binding efficiency. Fentanyla synthetic opioid analgesic approximately 50 to 100 times more potent than morphine is frequently cited as the benchmark for strength in modern palliative care. Unlike morphine, which is derived from the opium poppy, fentanyl is fully synthetic, allowing for precise manufacturing consistency.
Another contender in the high-potency arena is sufentanil, often reserved for surgical anesthesia rather than daily outpatient use. For long-term chronic pain management, methadone serves a dual purpose as both an analgesic and a maintenance therapy for opioid dependency. Hydrocodone and oxycodone are widely prescribed, yet they sit slightly below fentanyl in terms of milligram-for-milligram potency. Physicians calculate dosages based on "morphine equivalents" to switch patients safely between formulations without causing overdose or withdrawal symptoms.
The mechanism behind these drugs involves mimicking natural endorphins. They bind to mu-opioid receptors in the central nervous system. This binding inhibits the release of neurotransmitters responsible for sending pain signals to the brain. The stronger the binding affinity, the less mass of the drug is required to achieve effect. This concentration factor creates the primary danger zone for accidental exposure.
| Medication | Potency Relative to Morphine | Common Administration Routes | Primary Medical Use |
|---|---|---|---|
| Fentanyl | 50-100x | Transdermal patch, Buccal tablet | Cancer pain, Chronic severe pain |
| Morphine | 1x (Baseline) | Oral, Intravenous | General severe pain control |
| Hydromorphone | 5-10x | Oral solution, Injection | Acute post-operative pain |
| Methadone | Variable | Oral tablets | Chronic pain, Addiction treatment |
Risk Factors and Safety Protocols
Prescribing the most powerful pain medication requires rigorous oversight. The body builds tolerance quickly, meaning a dose that works today might be insufficient tomorrow. This phenomenon forces patients to increase dosages under strict supervision, creating a pathway toward physiological dependence. Dependence is a normal biological response to chronic opioid use, distinct from addiction, which involves compulsive behavior despite harm.
Respiratory depression remains the most critical safety concern. At very high doses, these medications can slow breathing to fatal levels. To mitigate this, many regions mandate carrying naloxone alongside prescriptions. Naloxone acts as an emergency antagonist, reversing opioid effects within minutes. It is a life-saving tool that allows for safer administration of high-potency therapies.
Regulatory bodies classify these drugs as controlled substances. In Ireland and the UK, they fall under the Misuse of Drugs Act, restricting who can prescribe and dispense them. Pharmacists require specific licenses to stock certain formulations. This prevents diversion to illicit markets, though counterfeit pills remain a public health threat globally.
Alternative Pathways for Extreme Discomfort
Opioids are not the only option for managing debilitating pain. Interventional techniques sometimes bypass the gastrointestinal tract entirely. Neuromodulation devices can target nerve pathways directly. Spinal cord stimulation uses electrical currents to mask pain signals before they reach the brain. Epidural injections deliver concentrated medication directly around the spinal nerves.
Ketamine infusion therapy has gained traction for complex regional pain syndromes. While technically an anesthetic, low-dose ketamine works on different receptors (NMDA) compared to opioids. This difference reduces the risk of cross-tolerance and respiratory depression. Multidisciplinary pain clinics often combine these physical interventions with psychological support. Cognitive behavioral therapy helps manage the emotional burden of living with constant pain, reducing the perceived intensity.

Navigating Conversations with Specialists
If your current regimen fails to control symptoms, bringing up escalation to a specialist is essential. You need evidence of failed attempts before a doctor considers stronger options. Keep a pain diary recording intensity scores, duration, and triggers. Show your doctor how pain impacts daily tasks like walking, sleeping, or working.
Be honest about side effects. Constipation and nausea are common with opioids, but sedation or confusion can signal overmedication. Never demand specific brand names; instead, describe the relief you need. Ask about non-pharmacological options that complement medication. A treatment plan should always include exit strategies, defining when and how to reduce dosage if health improves.
Signs That Warrant Immediate Attention
Recognizing adverse reactions is vital for anyone on high-intensity regimens. Pinpoint pupils, slurred speech, and excessive drowsiness indicate toxicity. These symptoms require immediate intervention, potentially involving emergency services. Distinguish between expected sedation at night versus dangerous grogginess during the day.
Monitoring interactions with other substances is equally important. Mixing opioids with alcohol or benzodiazepines dramatically increases overdose risk. Always inform your healthcare provider about all supplements and prescription drugs you take. Even seemingly harmless cold medicines containing antihistamines can compound sedative effects.
Is fentanyl always the strongest painkiller available?
While fentanyl is exceptionally potent for patient use, veterinarians use carfentanil which is significantly stronger. However, carfentanil is toxic for humans in tiny amounts and is not approved for treating human pain conditions. For medical practice, fentanyl patches represent the peak of transdermal delivery systems.
Can these medications cause addiction?
Yes, the risk exists regardless of dosage or intention. Physiological dependence occurs naturally, but addiction involves behavioral changes. Risk factors include personal history of substance abuse, mental health conditions, and taking higher doses than prescribed. Doctors monitor usage closely to minimize this risk.
How do doctors decide which opioid to prescribe?
Selection depends on pain type, renal function, and metabolism speed. Fentanyl patches suit stable round-the-clock pain. Immediate-release formulations work for breakthrough episodes. Patient age and liver health dictate whether extended-release versions are safe.
Are there legal restrictions on these drugs?
Strictly yes. They are Schedule II or Class B controlled substances depending on jurisdiction. Prescriptions require specific authorization forms, and pharmacies track inventory meticulously to prevent loss or theft. Transporting these across borders is heavily regulated.
What happens if I miss a dose of severe pain medication?
Missing a scheduled dose causes the medication levels to drop, triggering withdrawal symptoms like anxiety and sweating. Depending on the half-life of the drug, effects vary within hours. Contact your prescribing physician immediately to adjust the schedule safely without doubling up on doses later.